When pharmacy and medical benefits work together, outcomes improve and costs go down.
Rightway connects pharmacy and medical data in real-time to give our clinical team the full picture, delivering smarter guidance and measurably lower costs.

One platform. One team.
One connected care model.
Pharmacy and medical decisions don’t happen in isolation. Neither should your benefits.
How it works across the full care journey:
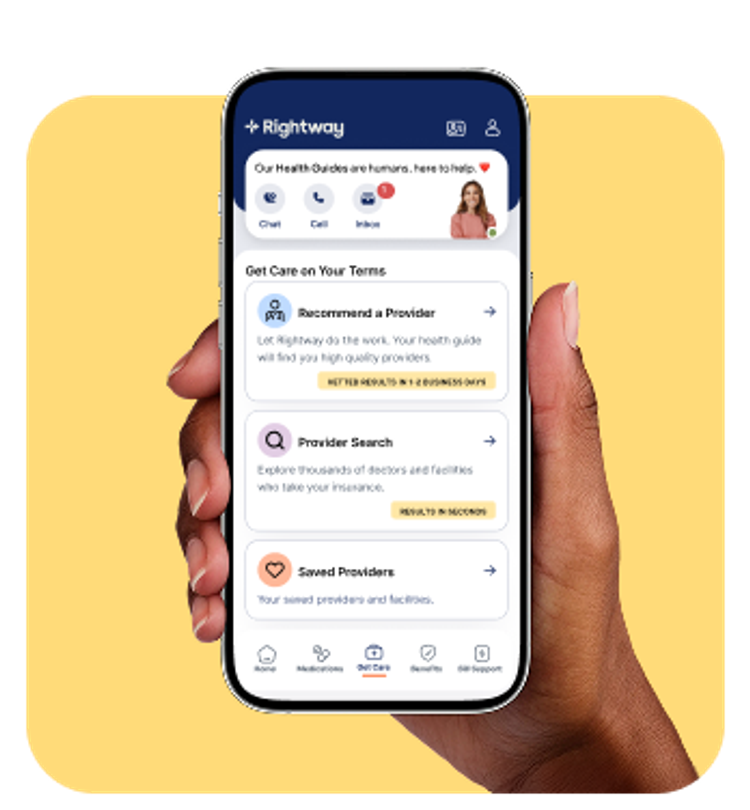
A connected clinical platform.
Righway’s Pharmacy Benefit Management (PBM) and care navigation solutions operate within a single clinical and technology platform.
Integrated medical and pharmacy data create a complete view of each member, so care and medication decisions are made with the full picture in mind.

Intelligence that drives action.
Medical and pharmacy data are continuously analyzed to identify gaps and cost drivers, triggering proactive outreach and clear next steps.

A truly coordinated clinical team.
Each member’s dedicated care team works from the same insights and acts together—eliminating handoffs, reducing delays, and aligning clinical and financial decisions around better outcomes and total cost of care.
- Pharmacists manage medication access, affordability, and prior authorizations, and coordinate with pharmacies and providers on the members behalf.
- Nurse-led teams guide members to the right providers and sites of care, and resolve billing, coverage, and referral issues.

A unified member experience.
Members access support through a single app—chatting with clinicians, searching medications and providers, viewing digital ID cards, and tracking out-of-pocket costs.

A complete view for employers.
Integrated medical and pharmacy data provide clear visibility into utilization trends, adherence, and site-of-care optimization—replacing fragmented reporting with actionable insight.
Connected care moments.
Maria stops refilling her diabetes medication.
Pharmacy data flags the gap. Our clinical team identifies side effects driving non-adherence, adjusts therapy, and aligns coverage—preventing complications and avoidable spend.
James isn’t improving on his current medication.
His care team analyze his medical and pharmacy history, coordinates with his provider to optimize therapy, and ensure seamless coverage, improving symptom control and reducing avoidable complications.
The best member experience. Period.
One front door. One coordinated care team. Zero runaround.
Members have a single place for every pharmacy and medical need, backed by a coordinated clinical team.
Clinical care teams deliver unmatched member service.
- On-demand, human-led care teams provide personalized support, actionable guidance, and expert education.
- Our team drives members towards the most appropriate, high-quality care and medications at the lowest costs.

“I can get issues resolved on a Sunday. Rightway PBM and care navigation work together so well. The pharmacy and care navigation teams work together when there is an issue. It just works.”MARK SCHAERRER,Vice President of HR at Verisys

Rightway does the heavy lifting.
Pharmacists, nurses, health guides, social workers, and billing specialists collaborate to deliver personalized, coordinated support, alleviate any confusion, and handle time-consuming tasks. Our team helps members:
A single app for medical and pharmacy needs.
- Intuitive mobile and web app simplifies access.
- Members can chat with their care team in real-time.
- Self-service access to high-quality, affordable providers, facilities, and medications.
- Members can track real-time progress towards deductible and out-of-pocket activity.
- Convenient access to healthcare insurance and pharmacy ID cards.
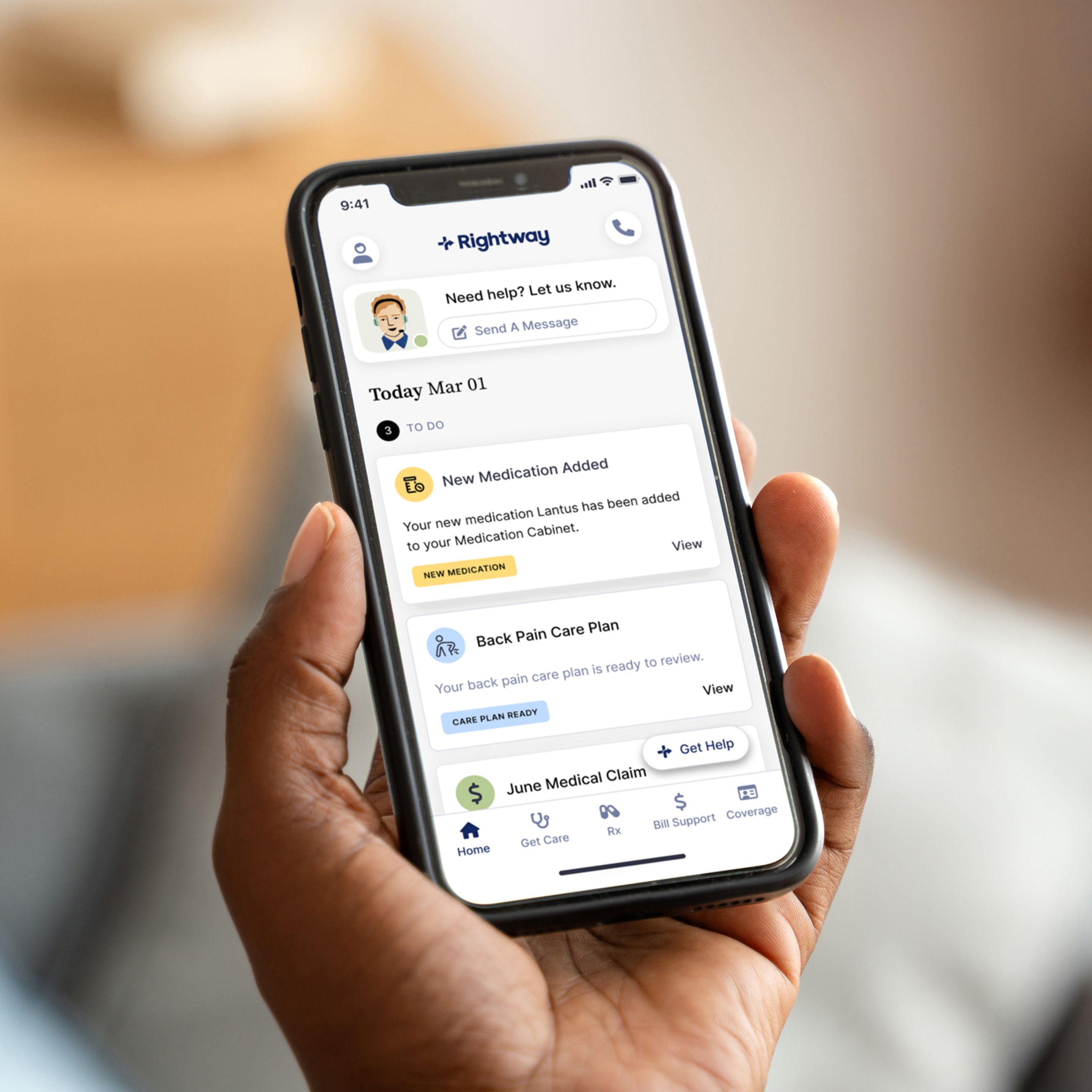
A true partner that lightens your load.
Smarter decisions.
Unified medical and pharmacy data with integrated reporting that connects spend, outcomes, and utilization in one view.
Streamlined partnership.
One partner for seamless account management and admin support protects your teams’ time.
High-touch implementation.
Full-spectrum support and smooth implementation that reduces the load on benefit teams and minimizes disruption for members.
Metrics that matter.
Frequently Asked Questions.
Does Rightway provide medical coverage or replace our health plan?
No. Rightway does not provide medical coverage or replace the medical plan. Members keep their existing health plan while Rightway administers and supports pharmacy benefits and care navigation.
How does Rightway work with existing plans and providers?
Members keep their current medical plan and can keep their existing providers, or opt into recommendations from the Rightway care team. We ingest their medical data directly from the plan sponsor, so our clinical team has the full picture from day one.
What changes are required to adopt Rightway?
None. Employers and members keep their current plans, providers, and pharmacy relationships. No plan changes or new workflows are required.
Can you integrate with third party programs?
Yes, we seamlessly coordinate with third-party programs.













