What is a pharmacy benefit manager (PBM)?
A pharmacy benefit manager (PBM) is a company that negotiates drug prices, determines coverage and processes prescription claims on behalf of employers. Their role is to manage prescription drug benefits to lower costs and improve access. By negotiating pricing and determining which options are covered, PBMs are deeply embedded in the healthcare system.
Since emerging in the 1960s as claims processors, PBMs have evolved into powerful middlemen controlling nearly every aspect of prescription drug pricing and access. Today, the largest 3 PBMs manage pharmacy benefits for over 270 million Americans, wielding enormous influence over the United States prescription drug market, according to the Federal Trade Commission.
But that influence has come with growing scrutiny. Many PBMs rely on complex pricing structures and revenue streams that can obscure true costs and misalign incentives. These practices have contributed to rising drug spend and increased pressure from regulators, employers and policymakers.
In this article, we’ll break down how PBMs make money, where traditional models create misalignment and what employers should look for in a more transparent, aligned approach to managing pharmacy benefits.
Key highlights:
- A pharmacy benefit manager (PBM) manages prescription drug pricing, coverage and access on behalf of employers.
- Traditional PBM models often rely on spread pricing, retained rebates and pharmacy ownership, creating misaligned incentives that drive up costs.
- Transparency alone isn’t enough. Many “transparent” and pass-through models still leave room for hidden profit and limited savings.
- Rightway’s fiduciary-aligned PBM removes these conflicts entirely, delivering 100% pass-through pricing, providing pharmacy navigation and consistently driving the lowest net cost.
Key roles and responsibilities of PBM solutions.
PBMs manage negotiations, clinical programs and administrative processes that influence medication availability, costs and access.
Formulary management.
A drug formulary is a list of covered medications organized into cost tiers that determine what a member pays. PBMs design and maintain formularies by evaluating clinical efficacy, safety and cost-effectiveness. However, formulary decisions can be influenced by manufacturer rebates rather than pure clinical value.
Drug price negotiation.
PBMs negotiate with pharmaceutical manufacturers to secure rebates and discounts in exchange for favorable formulary placement. These negotiations can generate substantial savings, but only if passed through to plan sponsors and members. Legacy PBMs often retain a portion of negotiated rebates, creating conflicts where higher list prices become more profitable.
Network design.
PBMs build and manage pharmacy networks by contracting with or owning retail, mail-order and specialty pharmacies. They determine which pharmacies members can access at preferred pricing and may steer patients toward pharmacies they own or operate. Network design has a direct impact on member convenience, medication adherence and employer costs.
Cost containment.
PBMs aim to prevent unnecessary spending through utilization management programs like prior authorization, step therapy and quantity limits. These clinical programs can protect employers from wasteful spending, but aggressive policies can also create barriers that frustrate members and prevent them from accessing the medications they need.
Claims processing.
PBMs operate the technological infrastructure that adjudicates pharmacy claims in real time, verifying eligibility, applying formulary rules and processing payments. This system processes billions of transactions annually.
How do pharmacy benefit managers work?
PBMs coordinate how prescription drugs are priced, accessed and paid for across employers, pharmacies and manufacturers. While the system can feel complex, it follows a defined process from plan design to dispensing and ongoing cost management.
1. Employers partner with a PBM to manage pharmacy benefits.
Employers contract with a PBM to administer their pharmacy benefit program. This includes setting up coverage rules, defining member cost-sharing and outsourcing the day-to-day management of prescription drug benefits.
The contract establishes how the program will operate, including pricing structure, service scope and performance expectations. From there, the PBM becomes responsible for managing both the financial and operational components of the pharmacy benefit.
Here’s how the partnership works:
- Employers work with PBMs to design and administer pharmacy benefits
- Contracts define fees, coverage structure and program rules
- PBMs take on operational responsibility for managing prescription benefits
2. PBMs design formularies and negotiate drug pricing.
PBMs build formularies, which are lists of covered medications organized into tiers that determine what members pay. These formularies influence generic drug pricing and specialty drug availability, and are developed using clinical review, cost considerations and market dynamics.
At the same time, PBMs negotiate pricing with drug manufacturers and pharmacies. This includes rebates, discounts and contracted rates. Together, these decisions directly shape both what medications members can access and how much the plan ultimately spends.
Here’s how pricing and coverage are determined:
- Formularies define which medications are covered and at what tier
- PBMs negotiate pricing and discounts with manufacturers and pharmacies
- Generic and brand drug pricing both influence total plan costs
3. Pharmacies dispense medications based on PBM rules.
When a member fills a prescription, the pharmacy processes it in accordance with the PBM’s rules. This includes checking formulary coverage, applying any utilization requirements and confirming network eligibility.
PBMs also establish pharmacy networks, which determine where members can fill prescriptions. These networks can include retail, mail-order and specialty pharmacies, and may also include pharmacies owned or operated by the PBM.
Here’s how members access prescriptions:
- Pharmacies follow PBM-defined coverage and eligibility rules
- Network design determines which pharmacies members can access
- Dispensing is guided by formulary placement and utilization requirements
4. Claims are processed and payments are reconciled.
After the sale, the PBM adjudicates the claim. This process verifies eligibility, applies pricing rules and determines how costs are split between the member and the employer plan.
Once the claim is processed, the PBM facilitates payment—collecting funds from the plan sponsor and reimbursing the pharmacy. This step ensures all parties are paid according to the agreed pricing structure.
Here’s how the money flows:
- Claims are processed when a prescription is filled
- Member cost and plan cost are calculated at the point of sale
- PBMs manage payment flow between employers, pharmacies and other parties
5. PBMs manage utilization and optimize ongoing costs.
Beyond individual transactions, PBMs manage how medications are used over time. This includes programs like prior authorization, step therapy and quantity limits, which are designed to ensure appropriate use and control unnecessary spending.
PBMs also monitor claims data and prescribing patterns to identify trends and opportunities for cost management. These insights help employers adjust their benefit design and manage pharmacy spend over time.
Here’s how costs are managed over time:
- Utilization management programs guide appropriate medication use
- PBMs monitor trends and analyze claims data
- Ongoing adjustments help manage long-term pharmacy costs
Who interacts with a PBM solution?
The role of PBMs puts them at the center of a complex web of relationships connecting everyone involved in prescription drug access and pricing.
Plan sponsors.
Employers contract with PBMs to administer pharmacy benefit programs to their employees, outsourcing negotiating prices, managing formularies and processing claims. Without transparent contracts and pass-through pricing, plan sponsors often lack visibility into where their pharmacy dollars actually go.
Drug manufacturers.
Pharmaceutical companies negotiate rebate agreements with PBMs in exchange for favorable formulary placement. Legacy PBMs may favor higher-priced medications that generate larger rebates, driving up spending and contributing to skyrocketing drug prices.
Pharmacies.
Retail and specialty pharmacies contract with PBMs to fill prescriptions, accepting reimbursement rates negotiated by the PBM. These rates often include pricing formulas that can leave pharmacies operating at thin margins. PBM-owned pharmacies may receive preferential rates or steering mechanisms that disadvantage competitors.
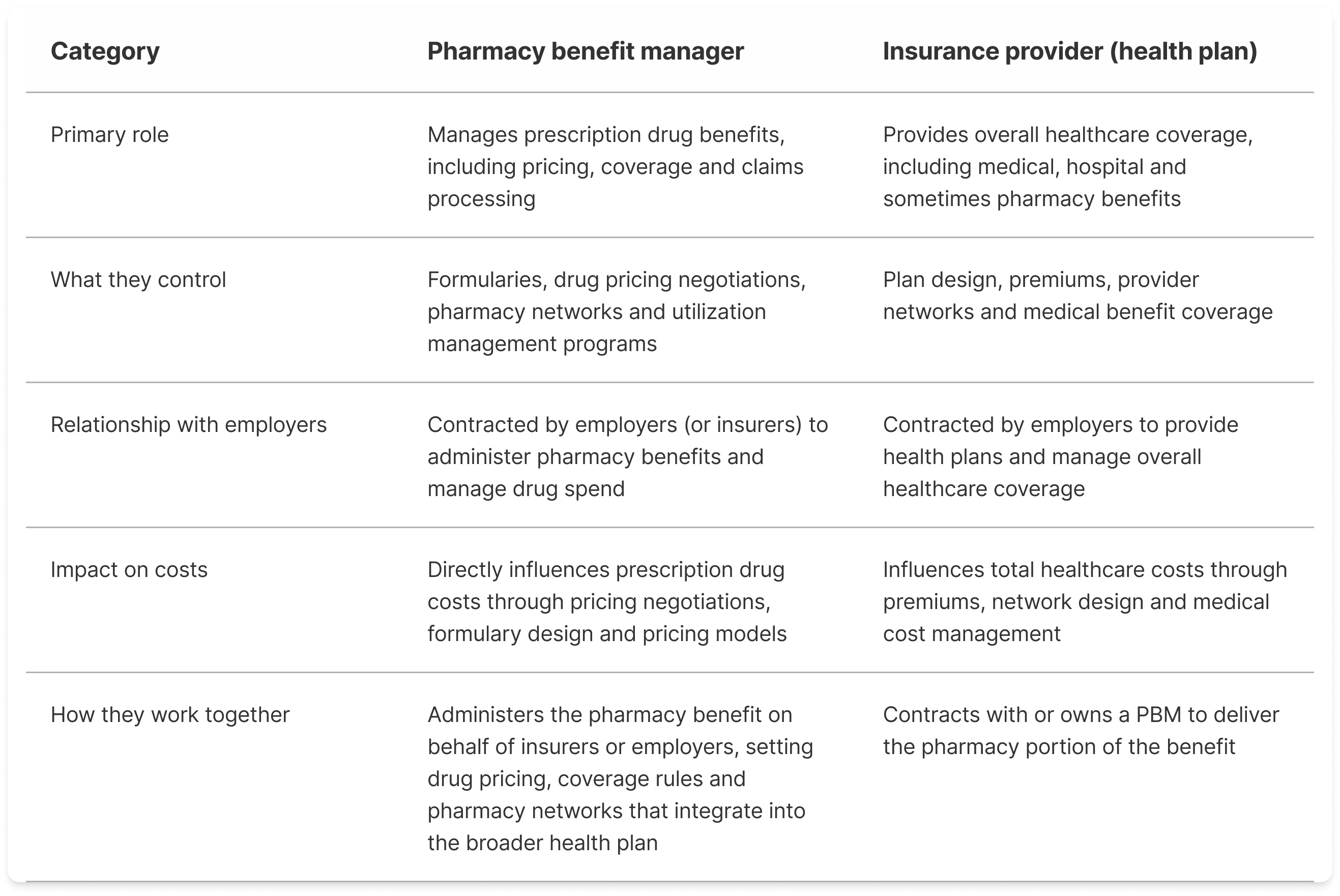
PBM vs insurance: What’s the difference?
Pharmacy benefit managers and health insurance providers play distinct but interconnected roles in managing healthcare benefits. While insurers oversee overall medical coverage, PBMs focus specifically on prescription drug benefits by working behind the scenes to influence pricing, access and utilization.
Here’s how they compare:
How do PBMs make money? Revenue streams explained.
PBMs earn revenue through multiple streams—some transparent, others opaque and misaligned with client interests. Traditional PBMs inflate list prices, steer members into their own pharmacies and manipulate rebate structures to make "savings" appear larger while costs keep rising.
Rebates and manufacturer fees.
Pharmaceutical manufacturers pay PBMs rebates to secure favorable formulary placement. These payments create powerful incentives to favor high-rebate medications over lower-cost alternatives. In traditional PBM contracts, a significant portion of rebates may be retained rather than passed through to the plan sponsor.
Spread pricing.
Spread pricing occurs when a PBM charges the plan sponsor more for a medication than it reimburses the pharmacy, pocketing the difference as profit. Studies showed that the big 3 PBMs generated an estimated $1.4 billion of income from spread pricing, according to the FTC.
Administrative fees.
PBMs charge administrative fees for services like claims processing and formulary management. Percentage-based fees tied to drug spend create hidden costs and conflicts similar to spread pricing, while fixed fees (per-member-per-month) are predictable.
Mail order and specialty margins.
Many traditional PBMs own mail-order and specialty pharmacies, creating opportunities to profit from both PBM services and pharmacy dispensing. They may steer patients toward their own pharmacies, prioritizing profits over member choice.
PBM pricing models.
The way a PBM’s drug pricing is structured determines whether its incentives align with yours or work against you. Here are the four main models:
1. Traditional PBM model.
Traditional PBM models, like the Big 3, have long been the standard in pharmacy benefit management. However, their opaque practices, hidden fees and profit-driven incentives have come under scrutiny for inflating drug costs.
These models prioritize their profits by boosting prices, favoring high rebate medications, controlling pharmacy networks for additional revenue and manipulating classifications—all at the expense of plan sponsors and members.
2. Transparent PBM model.
Transparent PBMs emerged as a response to widespread criticism of the traditional PBM model, which has been opaque about pricing, rebates and fees. This lack of transparency created mistrust, leading to the demand for a model that allowed clients to see the full financial picture of their pharmacy benefit plans.
These models address these concerns by offering more visibility into how money flows through the pharmacy benefit process. They improve visibility into pricing and fees, giving employers more insight, but they may not pass through rebates and savings. Potential conflicts prevent them from fully aligning with employer goals, limiting the overall savings impact.
3. Pass-through PBM model.
Pass-through PBMs ensure that all cost savings, rebates and negotiated discounts flow directly to the client without being retained by the PBM. This model was created in response to practices that inflate pharmacy spend, like spread pricing in traditional PBMs.
While pass-through PBMs aim to provide transparency and improve value by returning all savings to employers, many operate as hybrids, limiting their actual transparency and cost savings. Their focus on price alone and potential channel steering may reduce their effectiveness in truly lowering overall healthcare costs for employers.
4. Aligned PBM model.
Aligned PBMs go beyond transparent and pass-through models and align their operations with the employer’s goals. To be fully aligned, every initiative of the PBM must serve the employer’s needs, which are usually to lower costs, give their teams high-quality benefits and improve health outcomes for their populations.
These PBMs provide transparent contracts and avoid conflicts of interest, like owning pharmacies or manufacturing their own costly biosimilars. Aligned solutions are the most effective choice for employers, offering total cost transparency and a commitment to health outcomes. With no conflicts from pharmacy ownership, they deliver real cost savings and improved care for employees.
Pros and cons of pharmacy benefit management for employers.
PBMs promise to simplify administration and control pharmacy spending. When operating transparently with aligned incentives, they can deliver significant value. However, many plan sponsors are dissatisfied with their PBM contracts, highlighting significant drawbacks to certain models.
Benefits of PBMs.
When aligned with employer and member needs, PBMs provide substantial value through:
- Cost management through scale: Leveraging purchasing power to negotiate lower prices and rebates.
- Administrative work: Handling complex pharmacy operations, including claims processing and network management.
- Clinical oversight: Promoting cost-effective medication use through formulary management and utilization programs.
- Network optimization: Building pharmacy networks that balance access, convenience and cost.
- Data analytics: Providing reporting tools that help identify cost drivers and optimize benefit design.
Drawbacks of PBMs.
Traditional, misaligned PBM models have significant pain points for employers:
- Opaque pricing: Spread pricing, retained rebates and hidden fees make it impossible to understand or control true costs.
- Conflicts of interest: When PBMs profit from higher drug costs or owned pharmacies they steer members toward, their incentives oppose employer goals.
- Limited visibility: Lack of transparency prevents accountability.
- Market concentration: The three largest PBMs control over 80% of the market, reducing competition, according to the FTC.
- Misaligned incentives: When PBM revenue grows as drug costs rise, they have no reason to contain spending.
Choosing a trusted PBM partner.
Selecting the right PBM partner is one of the most important decisions employers make about their healthcare benefits strategy. Employers should look for:
Transparent, aligned pricing.
A truly transparent PBM operates with 0% supply chain ownership, 100% pass-through pricing and one flat admin fee. There are no games—no spread pricing, retained rebates, or hidden incentives. Every dollar saved flows directly back to clients and members.
Look for PBMs that provide fully auditable reporting, are fiduciary-aligned and tie their success to your outcomes through a total spend guarantee.
Embedded pharmacy navigation.
The best member experience comes from having expert guidance at every step. Pharmacy navigation delivered by licensed pharmacists and pharmacy technicians provides real-time support, guiding members to high-value care while handling complex tasks.
Members should be able to track prescriptions, compare prices, manage mail order and connect with pharmacy experts through an intuitive app.
Proven results.
Demand evidence of performance. Look for PBMs that demonstrate measurable cost savings through total PMPM spend guarantees backed by dollar-for-dollar accountability, improved clinical outcomes, including medication adherence and biosimilar adoption, high member satisfaction and seamless implementation.
Leading employers like Tyson Foods have transformed their pharmacy benefits by partnering with transparent PBMs that align incentives and deliver exceptional member experiences.
Simplify benefits management with Rightway.
Managing pharmacy benefits shouldn’t require navigating hidden fees, complex contracts, or unclear results. Rightway's transparent PBM solution is built to give employers a model that lowers total pharmacy spend while making costs easier to understand and control.
Our PBM operates with fully aligned pricing. There’s no spread pricing, no retained rebates and no competing financial incentives. Every dollar flows through to the plan, backed by a total spend guarantee that puts real accountability behind performance.
Beyond pricing, Rightway pairs its PBM with pharmacist-led navigation to guide members to the most effective, lowest-cost medications. From comparing options to resolving issues and managing ongoing therapy, our clinical team supports members at every step.
The result is a pharmacy benefit that is easier to manage, more predictable and designed to consistently deliver lower net cost.
Book a demo today and see how Rightway’s PBM solution can help simplify benefits management and improve healthcare outcomes for your employees.
Frequently asked questions.
Who are the largest PBMs?
The pharmacy benefits industry is a complex and opaque system dominated by the big three PBMs —CVS Caremark, OptumRx and Express Scripts. When combined with Humana, Prime Therapeutics and MedImpact, these six control 94% of the market, according to the FTC, solidifying their role as the primary gatekeepers in prescription drug pricing and access.
Their market dominance raises concerns about pricing power, conflicts of interest from vertical integration and reduced competition.
How does a PBM reduce drug costs?
PBMs reduce costs through negotiating manufacturer rebates, managing pharmacy networks, implementing utilization management programs and providing clinical programs. However, the actual savings employers realize depend entirely on the contract structure—traditional PBMs may retain much of these savings, while aligned PBMs with transparent, pass-through pricing ensure that all savings reach plan sponsors and members.
Why are PBMs controversial?
PBMs have become controversial due to business practices that prioritize profit over affordability, including spread pricing, retained rebates, pharmacy ownership, creating steering conflicts, lack of transparency and market concentration. These practices have drawn scrutiny from Congress and regulators.
What does PBM transparency mean?
PBM transparency means full disclosure of all costs, fees, rebates and financial arrangements. A transparent PBM provides auditable reporting showing exactly what the plan sponsor pays, what pharmacies receive and how the PBM is compensated.
How is Rightway different from legacy PBMs?
Rightway is the only PBM with pharmacy navigation delivered by licensed pharmacists and pharmacy technicians. Our team guides members to high-value medications and provides real-time support through our trusted app.
We operate with complete alignment—no supply chain ownership, hidden incentives, spread pricing, or rebate games. Instead, we deliver fully aligned pricing, 100% transparency and a total spend guarantee. What is spread pricing in pharmacy benefit management?
Are PBM solutions regulated?
Yes, PBM solutions are regulated at both the federal and state levels, but oversight varies widely. At the federal level, PBMs are subject to certain transparency and reporting requirements, while many states have introduced legislation to address pricing practices, rebate structures and pharmacy reimbursement.
For example, laws like Arkansas House Bill 1150 have been proposed to increase accountability and limit certain PBM practices. However, regulation is still evolving, and many employers continue to face limited visibility into how pharmacy dollars are managed.
What is a pass-through PBM?
A 100% pass-through PBM is a pricing model where the PBM passes all negotiated discounts, rebates and pharmacy payments directly to the employer without retaining a portion as profit. Instead, the PBM earns revenue through a fixed administrative fee.
This model is designed to improve transparency by removing hidden revenue streams like spread pricing. However, not all pass-through models operate the same way, and some may still include limitations or structures that impact total cost savings.
What makes a PBM partner truly aligned?
A truly aligned PBM operates with incentives that match the employer’s goals—lowering costs, improving outcomes and delivering a better member experience. This means eliminating financial structures that benefit from higher drug prices or increased utilization.
Aligned PBMs prioritize transparent pricing, avoid conflicts like pharmacy ownership and provide full visibility into costs and performance. Their success is tied directly to delivering measurable value, not increasing spend.